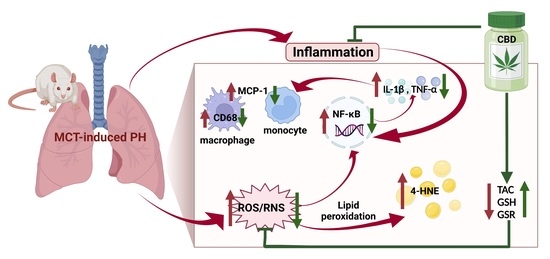
“Cannabinoid diphenol (CBD) is a non-toxic main component extracted from cannabis, which has the effects of anti-inflammatory, anti-apoptosis and anti-oxidative stress.
In recent years, exercise-induced myocardial injury has become a research hotspot in the field of sports medicine and sports physiology. Exercise-induced myocardial injury is closely related to oxidative stress, inflammatory response and apoptosis. However, there is no clear evidence of the relationship between CBD and exercise-induced myocardial injury.
In this study, by establishing an animal model of exhaustive exercise training in mice, the protective effect of CBD on myocardial injury in mice was elaborated, and the possible molecular mechanism was discussed.
After CBD intervention, the arrangement and rupture of myocardial fiber tissue and the degree of inflammatory cell infiltration were reduced, the deposition of collagen fibers in myocardial tissue decreased. CBD can also significantly inhibit cardiac hypertrophy. Meanwhile, the expression of IL-6, IL-10, TNF-α, Bax, Caspase-3, Bcl-2, MDA-5, IRE-1α, NOX-2, SOD-1, Keap1, Nrf2, HO-1, NF-κB and COX-2 was recovered to normal.
In addition, after CBD intervention, the protein expression of Keap1 was down-regulated, the translocation of Nrf2 from the cytoplasm to the nucleus was significantly increased, then the transcriptional activity was increased, and the expression of the downstream HO-1 antioxidant protein was increased, indicating that CBD may improve the cardiac function of exhaustive exercise training mice by activating Keap1/Nrf2/HO-1 signaling pathway. Molecular docking results also confirmed that CBD had a good binding effect with Keap1/Nrf2/HO-1 signaling pathway proteins.
In conclusion, the protective mechanism of CBD on myocardial injury in exhaustive exercise training mice may be to activate Keap1/Nrf2/HO-1 signaling pathway, and then exert anti-inflammatory, anti-apoptosis and inhibition of oxidative stress.”
https://pubmed.ncbi.nlm.nih.gov/35926578/
https://www.sciencedirect.com/science/article/abs/pii/S0009279722002848?via%3Dihub