
“Light-induced skin damage leads to cellular or molecular dysfunction, thus potentially causing different skin issues (e.g., skin aging, seborrheic dermatitis and pigmentation). Blue light, a potent visible light that was previously adopted for promoting skin regeneration, draws considerable concerns in the past several years due to their potential damage to the skins. In this work, we investigated the roles of blue light in skewing the functions of sebocytes – the major cells that compose the sebaceous gland – an important “active” neuro-immuno-endocrine organ in maintaining skin functions.
For therapeutically purposes, we employed cannabidiol (CBD), a clinically used non-psychotropic phytocannabinoid, to revert blue-light-induced sebocytes dysfunctions, including intracellular lipid secretion, inflammation, reactive oxygen species (ROS) secretion, and cell cycles. At the cellular level, CBD reduced the blue-light-enhanced intracellular lipid secretion, decreased inflammation, down-regulated intracellular ROS production, and restored the skewed cell cycles in the sebocytes. In the intracellular mechanism, CBD inhibited the blue-light-induced pro-apoptotic activity through rebalance BCL-2/BAX expression and down-regulated the NF-κB p65 pathway.
Collectively, this study demonstrated that CBD was a potent therapeutic agent for maintaining normal sebocytes functions, thus is a promising drug for skincare purposes, especially considering its effectiveness in restoring the twisted sebocytes behaviors.”



 “UV phototherapy used in chronic skin diseases causes redox imbalance and pro-inflammatory reactions, especially in the case of unchanged skin cells.
“UV phototherapy used in chronic skin diseases causes redox imbalance and pro-inflammatory reactions, especially in the case of unchanged skin cells. “Cannabidiol (CBD), a natural occurring phytocannabinoid, is used extensively in consumer products ranging from foods to shampoos, topical oils and lotions.
“Cannabidiol (CBD), a natural occurring phytocannabinoid, is used extensively in consumer products ranging from foods to shampoos, topical oils and lotions. “Psoriasis is associated with increased production of reactive oxygen species which leads to oxidative stress.
“Psoriasis is associated with increased production of reactive oxygen species which leads to oxidative stress.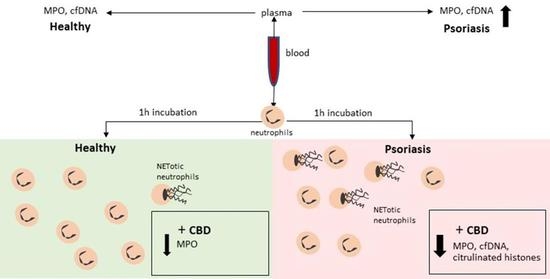
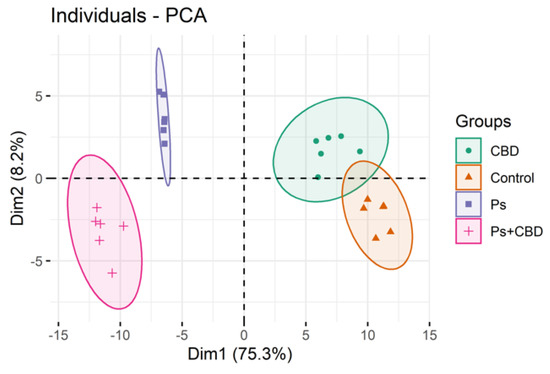
 “Psoriasis is a chronic inflammatory skin disease characterized by dysregulated keratinocyte differentiation, but oxidative stress also plays an important role in the pathogenesis of this disease.
“Psoriasis is a chronic inflammatory skin disease characterized by dysregulated keratinocyte differentiation, but oxidative stress also plays an important role in the pathogenesis of this disease. “The legalisation of
“The legalisation of