 “The anti-cancer effects of cannabinoids including CBD (Cannabidiol) and THC ((-)-trans-∆9-tetrahydrocannabinol) have been reported in the case of pancreatic cancer (PC).
“The anti-cancer effects of cannabinoids including CBD (Cannabidiol) and THC ((-)-trans-∆9-tetrahydrocannabinol) have been reported in the case of pancreatic cancer (PC).
The connection of these cannabinoids to KRas oncogenes that mutate in more than 90% of PC, and their effects on PD-L1, a key target of immune checkpoint blockade, have not been thoroughly investigated. Using cell lines and mouse models of PC, the effects of CBD and THC on cancer growth, the interaction between PC cells and a stromal cell, namely pancreatic stellate cells (PSCs), and the mechanism(s) involved were determined by cell-based assays and mouse study in vivo.
CBD and THC inhibited the proliferation of PC, PSC, and PSC-stimulated PC cells. They also suppressed pancreatic tumour growth in mice. Furthermore, CBD and/or THC reduced the expression of PD-L1 by either PC or PSC cells. Knockout of p-21 activated kinase 1 (PAK1, activated by KRas) in PC and PSC cells and, in mice, dramatically decreased or blocked these inhibitory effects of CBD and/or THC.
These results indicated that CBD and THC exerted their inhibitions on PC and PSC via a p-21 activated kinase 1 (PAK1)-dependent pathway, suggesting that CBD and THC suppress Kras activated pathway by targeting PAK1. The inhibition by CBD and THC of PD-L1 expression will enhance the immune checkpoint blockade of PC.”

 “Multiple therapeutic properties have been attributed to Cannabis sativa. However, further research is required to unveil the medicinal potential of Cannabis and the relationship between biological activity and chemical profile.
“Multiple therapeutic properties have been attributed to Cannabis sativa. However, further research is required to unveil the medicinal potential of Cannabis and the relationship between biological activity and chemical profile. “Objective: To determine the benefit of a tetrahydrocannabinol (THC)-rich cannabis oil on symptoms and quality of life of fibromyalgia patients.
“Objective: To determine the benefit of a tetrahydrocannabinol (THC)-rich cannabis oil on symptoms and quality of life of fibromyalgia patients. “Many people with MS (pwMS) use unregulated cannabis or cannabis products to treat the symptoms associated with the disease. In line with this, Sativex, a synthetic combination of cannabidiol (CBD) and Δ9-tetrahydrocannabinol (Δ9-THC) has been approved to treat symptoms of spasticity.
“Many people with MS (pwMS) use unregulated cannabis or cannabis products to treat the symptoms associated with the disease. In line with this, Sativex, a synthetic combination of cannabidiol (CBD) and Δ9-tetrahydrocannabinol (Δ9-THC) has been approved to treat symptoms of spasticity.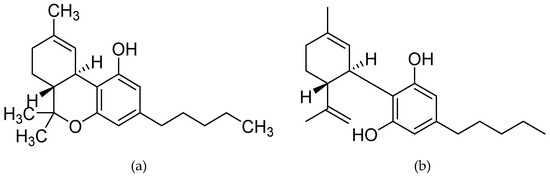
 “The prevalence of cancer pain will continue to rise as pain is common among the survivorship and general cancer population. As interest in cannabis and cannabinoids for medicinal use including pain management continues to rise, there is growing need to update and review the current state of evidence for their use. The literature was searched for articles in English with key words cannabis, cannabinoids, and cancer pain. The sources of articles were PubMed, Embase, and open Google search.
“The prevalence of cancer pain will continue to rise as pain is common among the survivorship and general cancer population. As interest in cannabis and cannabinoids for medicinal use including pain management continues to rise, there is growing need to update and review the current state of evidence for their use. The literature was searched for articles in English with key words cannabis, cannabinoids, and cancer pain. The sources of articles were PubMed, Embase, and open Google search. “Uterus transplantation is a complex surgical procedure. Uterine ischemia/reperfusion (IR) damage occurring in this process may cause loss of function in the uterus. Cell damage must be prevented for a healthy uterine function and successful transplantation.
“Uterus transplantation is a complex surgical procedure. Uterine ischemia/reperfusion (IR) damage occurring in this process may cause loss of function in the uterus. Cell damage must be prevented for a healthy uterine function and successful transplantation. “The purpose of this study was to examine the relationship between work-related injury and cannabis use in the past year.
“The purpose of this study was to examine the relationship between work-related injury and cannabis use in the past year. “In this proof-of-concept study, the antioxidant activity of phytocannabinoids, namely cannabidiol (CBD) and Δ9- tetrahydrocannabinol (THC), were investigated using an in vitro system of differentiated human neuronal SY-SH5Y cells.
“In this proof-of-concept study, the antioxidant activity of phytocannabinoids, namely cannabidiol (CBD) and Δ9- tetrahydrocannabinol (THC), were investigated using an in vitro system of differentiated human neuronal SY-SH5Y cells.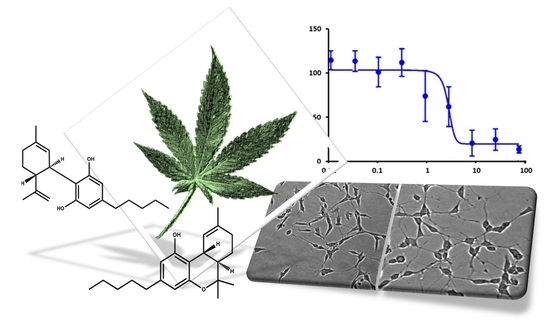
 “Evidence details how cannabis can influence the use of other psychoactive substances, including prescription medications, alcohol, tobacco and illicit drugs, but very little research has examined the factors associated with these changes in substance use patterns. This paper explores the self-reported use of cannabis as a substitute for alcohol among a Canadian medical cannabis patient population.
“Evidence details how cannabis can influence the use of other psychoactive substances, including prescription medications, alcohol, tobacco and illicit drugs, but very little research has examined the factors associated with these changes in substance use patterns. This paper explores the self-reported use of cannabis as a substitute for alcohol among a Canadian medical cannabis patient population. “Cannabis is a historical plant which has been used as a medicine in East Asia.
“Cannabis is a historical plant which has been used as a medicine in East Asia.