“HIV/SIV-associated oral mucosal disease/dysfunction (HAOMD) (gingivitis/periodontitis/salivary adenitis) represents a major comorbidity affecting HIV patients on anti-retroviral therapy.
“HIV/SIV-associated oral mucosal disease/dysfunction (HAOMD) (gingivitis/periodontitis/salivary adenitis) represents a major comorbidity affecting HIV patients on anti-retroviral therapy.
Using a systems biology approach, we investigated molecular changes (mRNA/microRNA) underlying HAOMD and its modulation by phytocannabinoids (delta-9-tetrahydrocannabinol (∆9-THC)) in uninfected (n = 5) and SIV-infected rhesus macaques untreated (VEH-untreated/SIV; n = 7) or treated with vehicle (VEH/SIV; n = 3) or ∆9-THC (THC/SIV; n = 3).
Relative to controls, fewer mRNAs were upregulated in THC/SIV compared to VEH-untreated/SIV macaques. Gene enrichment analysis showed differential enrichment of biological functions involved in anti-viral defense, Type-I interferon, Toll-like receptor, RIG-1 and IL1R signaling in VEH-untreated/SIV macaques. We focused on the anti-ER-stress anterior gradient-2 (AGR2), epithelial barrier protecting and anti-dysbiotic WAP Four-Disulfide Core Domain-2 (WFDC2) and glucocorticoid-induced anti-inflammatory TSC22D3 (TSC22-domain family member-3) that were significantly downregulated in oropharyngeal mucosa (OPM) of VEH-untreated/SIV macaques.
All three proteins localized to minor salivary gland acini and secretory ducts and showed enhanced and reduced expression in OPM of THC/SIV and VEH/SIV macaques, respectively. Additionally, inflammation associated miR-21, miR-142-3p and miR-29b showed significantly higher expression in OPM of VEH-untreated/SIV macaques. TSC22D3 was validated as a target of miR-29b.
These preliminary translational findings suggest that phytocannabinoids may safely and effectively reduce oral inflammatory responses in HIV/SIV and other (autoimmune) diseases.”
https://pubmed.ncbi.nlm.nih.gov/32630206/
https://www.mdpi.com/1999-4915/12/7/713
 “A post-antibiotic world is fast becoming a reality, given the rapid emergence of pathogens that are resistant to current drugs. Therefore, there is an urgent need to discover new classes of potent antimicrobial agents with novel modes of action.
“A post-antibiotic world is fast becoming a reality, given the rapid emergence of pathogens that are resistant to current drugs. Therefore, there is an urgent need to discover new classes of potent antimicrobial agents with novel modes of action.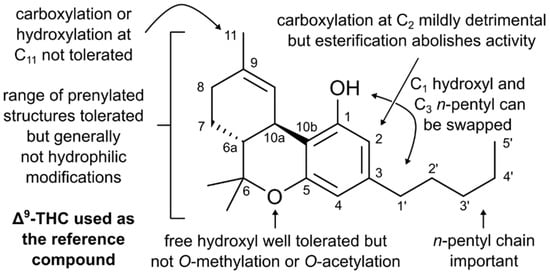


 “HIV/SIV-associated oral mucosal disease/dysfunction (HAOMD) (gingivitis/periodontitis/salivary adenitis) represents a major comorbidity affecting HIV patients on anti-retroviral therapy.
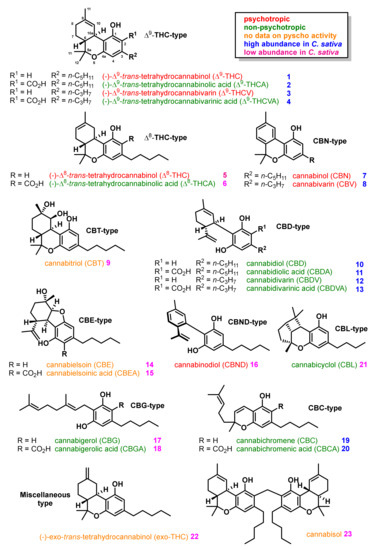
“HIV/SIV-associated oral mucosal disease/dysfunction (HAOMD) (gingivitis/periodontitis/salivary adenitis) represents a major comorbidity affecting HIV patients on anti-retroviral therapy. “Phytocannabinoids are bioactive natural products found in some flowering
“Phytocannabinoids are bioactive natural products found in some flowering  “Deposition of amyloid-beta (Aβ) peptide in the brain is the leading source of the onset and progression of Alzheimer’s disease (AD). Recent studies have suggested that anti-amyloidogenic agents may be a suitable therapeutic strategy for AD.
“Deposition of amyloid-beta (Aβ) peptide in the brain is the leading source of the onset and progression of Alzheimer’s disease (AD). Recent studies have suggested that anti-amyloidogenic agents may be a suitable therapeutic strategy for AD.

 “Objectives: To investigate the action of cannabinoids on spasticity and pain in secondary progressive multiple sclerosis, by means of neurophysiological indexes.
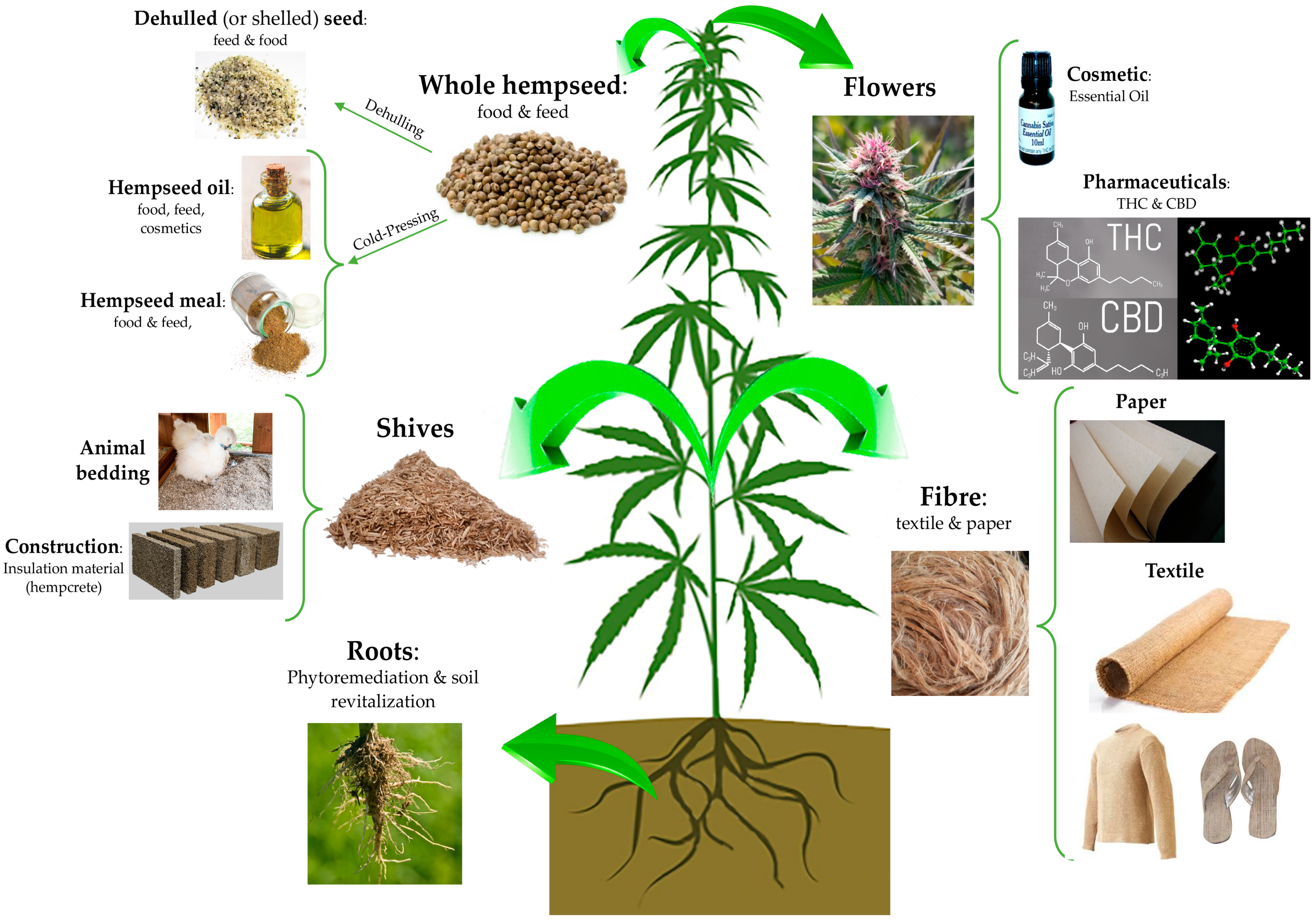
“Objectives: To investigate the action of cannabinoids on spasticity and pain in secondary progressive multiple sclerosis, by means of neurophysiological indexes. “Hempseeds, the edible fruits of the Cannabis sativa L. plant, were initially considered a by-product of the hemp technical fibre industry. Nowadays, following the restorationing of the cultivation of C. sativa L. plants containing an amount of delta-9-tetrahydrocannabinol (THC) <0.3% or 0.2% (industrial hemp) there is a growing interest for the hempseeds production due to their high nutritional value and functional features.
“Hempseeds, the edible fruits of the Cannabis sativa L. plant, were initially considered a by-product of the hemp technical fibre industry. Nowadays, following the restorationing of the cultivation of C. sativa L. plants containing an amount of delta-9-tetrahydrocannabinol (THC) <0.3% or 0.2% (industrial hemp) there is a growing interest for the hempseeds production due to their high nutritional value and functional features.