 “Deposition of amyloid-beta (Aβ) peptide in the brain is the leading source of the onset and progression of Alzheimer’s disease (AD). Recent studies have suggested that anti-amyloidogenic agents may be a suitable therapeutic strategy for AD.
“Deposition of amyloid-beta (Aβ) peptide in the brain is the leading source of the onset and progression of Alzheimer’s disease (AD). Recent studies have suggested that anti-amyloidogenic agents may be a suitable therapeutic strategy for AD.
Aim: The current review was proposed to address the beneficial effects of cannabis-based drugs for the treatment of AD, focusing primarily on Aβ modifications.
Result: A total of 17 studies were identified based on the inclusion criteria; however, nine studies qualified for this systematic review. The maximum and minimum cannabis dosages, mostly CBD and THC in animal studies, were 0.75 and 50 mg/kg, respectively. Cannabis (CBD and THC) was injected for 10 to 21 days. The findings of the 9 articles indicated that cannabis-based drugs might modulate Aβ modifications in several AD models.
Conclusion: Our findings establish that cannabis-based drugs inhibited the progression of AD by modulating Aβ modifications.”

 “Cannabinoids may have an important therapeutic potential for the treatment of dependence on crack cocaine.
“Cannabinoids may have an important therapeutic potential for the treatment of dependence on crack cocaine.

 “Acute Respiratory Distress Syndrome (ARDS) is a life-threatening complication that can ensue following Staphylococcus aureus infection. The enterotoxin produced by these bacteria (SEB) acts as a superantigen thereby activating a large proportion of T cells leading to cytokine storm and severe lung injury.
“Acute Respiratory Distress Syndrome (ARDS) is a life-threatening complication that can ensue following Staphylococcus aureus infection. The enterotoxin produced by these bacteria (SEB) acts as a superantigen thereby activating a large proportion of T cells leading to cytokine storm and severe lung injury. “Precise cannabis treatment dosing remains a major challenge, leading to physicians’ reluctance to prescribe medical cannabis.
“Precise cannabis treatment dosing remains a major challenge, leading to physicians’ reluctance to prescribe medical cannabis. “The seed of the hemp plant (Cannabis sativa L.) has been revered as a nutritional resource in Old World Cultures. This has been confirmed by contemporary science wherein hempseed oil (HSO) was found to exhibit a desirable ratio of omega-6 and omega-3 polyunsaturated fatty acids (PUFAs) considered optimal for human nutrition. HSO also contains gamma-linoleic acid (GLA) and non-psychoactive cannabinoids, which further contribute to its’ potential bioactive properties. Herein, we present the kinetics of the thermal stability of these nutraceutical compounds in HSO, in the presence of various antioxidants (e.g. butylated hydroxytoluene, alpha-tocopherol, and ascorbyl palmitate). We focussed on oxidative changes in fatty acid profile and acidic cannabinoid stability when HSO was heated at different temperatures (25 °C to 85 °C) for upto 24 h. The fatty acid composition was evaluated using both GC/MS and 1H-NMR, and the cannabinoids profile of HSO was obtained using both HPLC-UV and HPLC/MS methods. The predicted half-life (DT50) for omega-6 and omega-3 PUFAs in HSO at 25 °C was about 3 and 5 days, respectively; while that at 85 °C was about 7 and 5 hours respectively, with respective activation energies (Ea) being 54.78 ± 2.36 and 45.02 ± 2.87 kJ/mol. Analysis of the conjugated diene hydroperoxides (CDH) and p-Anisidine value (p-AV) revealed that the addition of antioxidants significantly (p < 0.05) limited lipid peroxidation of HSO in samples incubated at 25-85 °C for 24 h. Antioxidants reduced the degradation constant (k) of PUFAs in HSO by upto 79%. This corresponded to a significant (p < 0.05) increase in color stability and pigment retention (chlorophyll a, chlorophyll b and carotenoids) of heated HSO. Regarding the decarboxylation kinetics of cannabidiolic acid (CBDA) in HSO, at both 70 °C and 85 °C, CBDA decarboxylation led to predominantly cannabidiol (CBD) production. The half-life of CBDA decarboxylation (originally 4 days) could be increased to about 17 days using tocopherol as an antioxidant. We propose that determining acidic cannabinoids decarboxylation kinetics is a useful marker to measure the shelf-life of HSO. The results from the study will be useful for researchers looking into the thermal treatment of hempseed oil as a functional food product, and those interested in the decarboxylation kinetics of the acidic cannabinoids.”
“The seed of the hemp plant (Cannabis sativa L.) has been revered as a nutritional resource in Old World Cultures. This has been confirmed by contemporary science wherein hempseed oil (HSO) was found to exhibit a desirable ratio of omega-6 and omega-3 polyunsaturated fatty acids (PUFAs) considered optimal for human nutrition. HSO also contains gamma-linoleic acid (GLA) and non-psychoactive cannabinoids, which further contribute to its’ potential bioactive properties. Herein, we present the kinetics of the thermal stability of these nutraceutical compounds in HSO, in the presence of various antioxidants (e.g. butylated hydroxytoluene, alpha-tocopherol, and ascorbyl palmitate). We focussed on oxidative changes in fatty acid profile and acidic cannabinoid stability when HSO was heated at different temperatures (25 °C to 85 °C) for upto 24 h. The fatty acid composition was evaluated using both GC/MS and 1H-NMR, and the cannabinoids profile of HSO was obtained using both HPLC-UV and HPLC/MS methods. The predicted half-life (DT50) for omega-6 and omega-3 PUFAs in HSO at 25 °C was about 3 and 5 days, respectively; while that at 85 °C was about 7 and 5 hours respectively, with respective activation energies (Ea) being 54.78 ± 2.36 and 45.02 ± 2.87 kJ/mol. Analysis of the conjugated diene hydroperoxides (CDH) and p-Anisidine value (p-AV) revealed that the addition of antioxidants significantly (p < 0.05) limited lipid peroxidation of HSO in samples incubated at 25-85 °C for 24 h. Antioxidants reduced the degradation constant (k) of PUFAs in HSO by upto 79%. This corresponded to a significant (p < 0.05) increase in color stability and pigment retention (chlorophyll a, chlorophyll b and carotenoids) of heated HSO. Regarding the decarboxylation kinetics of cannabidiolic acid (CBDA) in HSO, at both 70 °C and 85 °C, CBDA decarboxylation led to predominantly cannabidiol (CBD) production. The half-life of CBDA decarboxylation (originally 4 days) could be increased to about 17 days using tocopherol as an antioxidant. We propose that determining acidic cannabinoids decarboxylation kinetics is a useful marker to measure the shelf-life of HSO. The results from the study will be useful for researchers looking into the thermal treatment of hempseed oil as a functional food product, and those interested in the decarboxylation kinetics of the acidic cannabinoids.” “The efficacy of cannabidiol (CBD) with and without concomitant clobazam (CLB) was evaluated in stratified analyses of four large randomized controlled trials, two in Lennox-Gastaut syndrome and two in Dravet syndrome.
“The efficacy of cannabidiol (CBD) with and without concomitant clobazam (CLB) was evaluated in stratified analyses of four large randomized controlled trials, two in Lennox-Gastaut syndrome and two in Dravet syndrome. “The Cannabis plant contains numerous components, including cannabinoids and other active molecules. The phyto-cannabinoid activity is mediated by the endocannabinoid system. Cannabinoids affect the nervous system and play significant roles in the regulation of the immune system.
“The Cannabis plant contains numerous components, including cannabinoids and other active molecules. The phyto-cannabinoid activity is mediated by the endocannabinoid system. Cannabinoids affect the nervous system and play significant roles in the regulation of the immune system.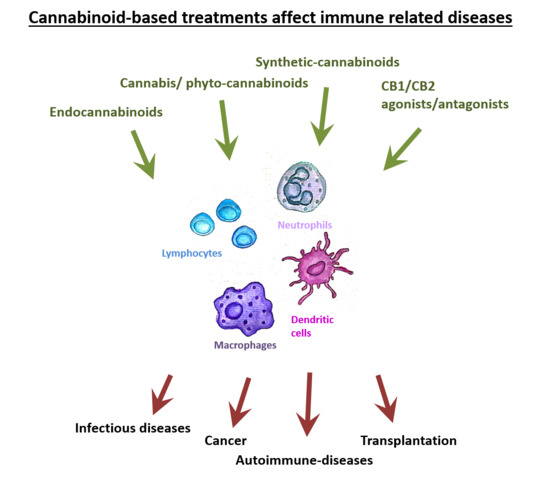
 “Current antiepileptic drugs (AEDs) are undesirable for many reasons including the inability to reduce seizures in certain types of epilepsy, such as Dravet syndrome (DS) where in one-third of patients does not respond to current AEDs, and severe adverse effects that are frequently experienced by patients.
“Current antiepileptic drugs (AEDs) are undesirable for many reasons including the inability to reduce seizures in certain types of epilepsy, such as Dravet syndrome (DS) where in one-third of patients does not respond to current AEDs, and severe adverse effects that are frequently experienced by patients.