 “Colorectal cancer (CRC) has a high mortality rate and is one of the most difficult diseases to manage due to tumour resistance and metastasis. The treatment of choice for CRC is reliant on the phase and time of diagnosis. Despite several conventional treatments available to treat CRC (surgical excision, chemo-, radiation- and immune-therapy), resistance is a major challenge, especially if it has metastasized. Additionally, these treatments often cause unwanted adverse side effects and so it remains imperative to investigate, alternative combination therapies.
“Colorectal cancer (CRC) has a high mortality rate and is one of the most difficult diseases to manage due to tumour resistance and metastasis. The treatment of choice for CRC is reliant on the phase and time of diagnosis. Despite several conventional treatments available to treat CRC (surgical excision, chemo-, radiation- and immune-therapy), resistance is a major challenge, especially if it has metastasized. Additionally, these treatments often cause unwanted adverse side effects and so it remains imperative to investigate, alternative combination therapies.
Photodynamic Therapy (PDT) is a promising treatment modality for the primary treatment of CRC, since it is non-invasive, has few side effects and selectively damages only cancerous tissues, leaving adjacent healthy structures intact. PDT involves three fundamentals: a Photosensitizer (PS) drug localized in tumour tissues, oxygen and light. Upon PS excitation using a specific wavelength of light, an energy transfer cascade occurs, that ultimately yields cytotoxic species, which in turn induces cell death.
Cannabidiol (CBD) is a cannabinoid compound derived from the Cannabis sativa plant, which is found to exert anticancer effects on CRC through different pathways, inducing apoptosis and so inhibits tumour metastasis and secondary spread.
This review paper highlights current conventional treatment modalities for CRC and their limitations, as well as discusses the necessitation for further investigation into unconventional active nanoparticle targeting PDT treatments for enhanced primary CRC treatment. This can be administered in combination with CBD, to prevent CRC secondary spread and so enhance the synergistic efficacy of CRC treatment outcomes, with less side effects.”

 “Exemestane is one of the aromatase inhibitors (AI) used as first line treatment for estrogen-receptor positive breast cancer in post-menopausal women. Exemestane acts by inhibiting aromatase, the enzyme responsible for the conversion of androgens to estrogens and also by promoting apoptosis of breast cancer cells. Nevertheless, despite its therapeutic success, this AI, after prolonged treatment, can induce acquired resistance, which causes tumor relapse. Therefore, it is important to find new strategies to overcome resistance in order to improve breast cancer treatment.
“Exemestane is one of the aromatase inhibitors (AI) used as first line treatment for estrogen-receptor positive breast cancer in post-menopausal women. Exemestane acts by inhibiting aromatase, the enzyme responsible for the conversion of androgens to estrogens and also by promoting apoptosis of breast cancer cells. Nevertheless, despite its therapeutic success, this AI, after prolonged treatment, can induce acquired resistance, which causes tumor relapse. Therefore, it is important to find new strategies to overcome resistance in order to improve breast cancer treatment. “Despite the constant development of new antiepileptic drugs (AEDs), more than 30% of patients develop refractory epilepsy (RE) characterized by a multidrug-resistant (MDR) phenotype. The “transporters hypothesis” indicates that the mechanism of this MDR phenotype is the overexpression of ABC transporters such as P-glycoprotein (P-gp) in the neurovascular unit cells, limiting access of the AEDs to the brain.
“Despite the constant development of new antiepileptic drugs (AEDs), more than 30% of patients develop refractory epilepsy (RE) characterized by a multidrug-resistant (MDR) phenotype. The “transporters hypothesis” indicates that the mechanism of this MDR phenotype is the overexpression of ABC transporters such as P-glycoprotein (P-gp) in the neurovascular unit cells, limiting access of the AEDs to the brain. “Cannabis has been used for thousands of years in many cultures for the treatment of several ailments including pain.
“Cannabis has been used for thousands of years in many cultures for the treatment of several ailments including pain. “Considering data from in vitro and in vivo studies,
“Considering data from in vitro and in vivo studies,  “Over the last decades a renewed interest in n-3 very long polyunsaturated fatty acids (PUFAs), derived mainly from fish oils in the human diet, has been observed because of their potential effects against cancer diseases, including breast carcinoma. These n-3 PUFAs mainly consist of eicosapentaenoic acid (EPA) and docosahexaenoic acid (DHA) that, alone or in combination with anticancer agents, induce cell cycle arrest, autophagy, apoptosis, and tumor growth inhibition. A large number of molecular targets of n-3 PUFAs have been identified and multiple mechanisms appear to underlie their antineoplastic activities. Evidence exists that EPA and DHA also elicit anticancer effects by the conversion to their corresponding ethanolamide derivatives in cancer cells, by binding and activation of different receptors and distinct signaling pathways. Other conjugates with serotonin or dopamine have been found to exert anti-inflammatory activities in breast tumor microenvironment, indicating the importance of these compounds as modulators of tumor epithelial/stroma interplay. The objective of this review is to provide a general overview and an update of the current n-3 PUFA derivative research and to highlight intriguing aspects of the potential therapeutic benefits of these low-toxicity compounds in breast cancer treatment and care.”
“Over the last decades a renewed interest in n-3 very long polyunsaturated fatty acids (PUFAs), derived mainly from fish oils in the human diet, has been observed because of their potential effects against cancer diseases, including breast carcinoma. These n-3 PUFAs mainly consist of eicosapentaenoic acid (EPA) and docosahexaenoic acid (DHA) that, alone or in combination with anticancer agents, induce cell cycle arrest, autophagy, apoptosis, and tumor growth inhibition. A large number of molecular targets of n-3 PUFAs have been identified and multiple mechanisms appear to underlie their antineoplastic activities. Evidence exists that EPA and DHA also elicit anticancer effects by the conversion to their corresponding ethanolamide derivatives in cancer cells, by binding and activation of different receptors and distinct signaling pathways. Other conjugates with serotonin or dopamine have been found to exert anti-inflammatory activities in breast tumor microenvironment, indicating the importance of these compounds as modulators of tumor epithelial/stroma interplay. The objective of this review is to provide a general overview and an update of the current n-3 PUFA derivative research and to highlight intriguing aspects of the potential therapeutic benefits of these low-toxicity compounds in breast cancer treatment and care.” “There is concern that recreational marijuana legalization (RML) may lead to increased
“There is concern that recreational marijuana legalization (RML) may lead to increased 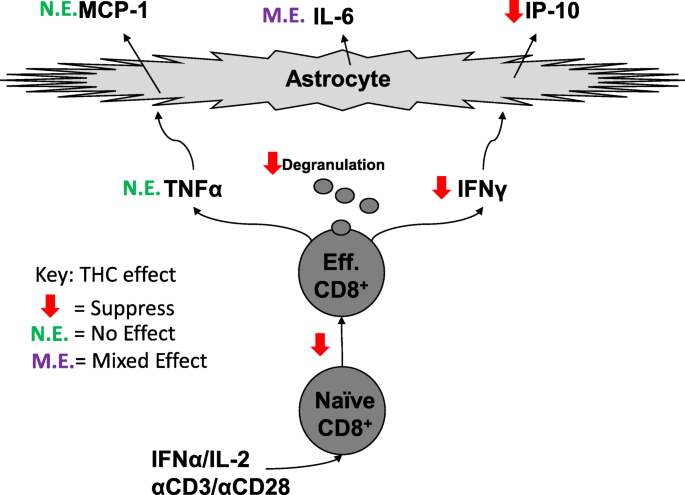 “CD8+ T cells can contribute to neuroinflammation by secretion of inflammatory cytokines like interferon γ (IFNγ) and tumor necrosis factor α (TNFα). Astrocytes, a glial cell in the brain, can be stimulated by IFNγ and TNFα to secrete the inflammatory cytokines, monocyte chemotactic protein 1 (MCP-1), interleukin 6 (IL-6), and interferon-γ inducible protein 10 (IP-10).
“CD8+ T cells can contribute to neuroinflammation by secretion of inflammatory cytokines like interferon γ (IFNγ) and tumor necrosis factor α (TNFα). Astrocytes, a glial cell in the brain, can be stimulated by IFNγ and TNFα to secrete the inflammatory cytokines, monocyte chemotactic protein 1 (MCP-1), interleukin 6 (IL-6), and interferon-γ inducible protein 10 (IP-10). “Cannabis benefits patients with inflammatory bowel disease (IBD).
“Cannabis benefits patients with inflammatory bowel disease (IBD).